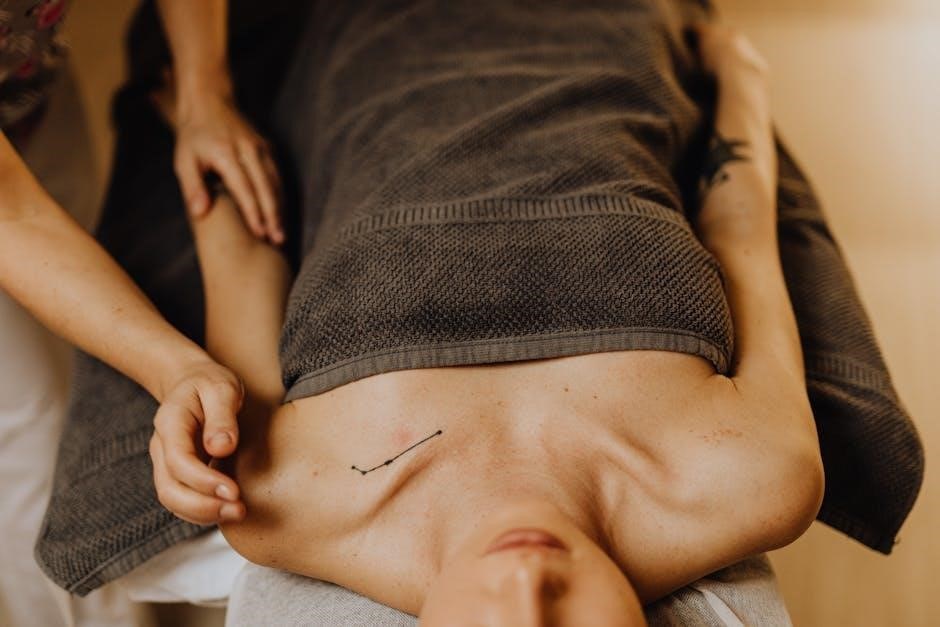
Understanding when not to utilize MLD is crucial for safety․ Certain health conditions present risks, demanding careful consideration before attempting lymphatic support techniques․
What is Manual Lymphatic Drainage?
Manual Lymphatic Drainage (MLD) is a gentle, specialized massage technique designed to encourage the natural drainage of the lymph, a vital fluid carrying waste products and immune cells․ Unlike traditional massage, MLD employs light rhythmic strokes and pressures along the lymphatic pathways․ This carefully orchestrated approach aims to stimulate lymphatic circulation, reducing swelling and supporting the body’s detoxification processes․
However, it’s not a universally suitable therapy․ Recognizing contraindications – conditions where MLD should be avoided – is paramount․ While often presented as a luxurious spa treatment, its physiological effects necessitate caution․ The technique’s impact on fluid movement means it can exacerbate certain health issues․ Therefore, a thorough understanding of these limitations is essential for both practitioners and individuals considering MLD to ensure safe and effective application, avoiding potential harm․
The Lymphatic System: A Brief Overview
The lymphatic system is a critical network of vessels, tissues, and organs responsible for maintaining fluid balance and supporting immune function․ It drains excess fluid from bodily tissues, filtering it through lymph nodes which contain immune cells․ This system plays a vital role in removing waste and fighting infection․ Understanding its delicate nature is key when considering interventions like Manual Lymphatic Drainage (MLD)․

Because MLD directly influences this system, certain conditions create contraindications․ The lymphatic system’s role in spreading infection means MLD could worsen acute illnesses․ Similarly, its connection to cardiovascular health necessitates caution with conditions like congestive heart failure․ Recognizing these interactions highlights why a comprehensive health assessment is crucial before initiating MLD, ensuring the therapy complements, rather than compromises, overall well-being and avoids potential complications․

Absolute Contraindications for MLD
Certain conditions strictly prohibit MLD application․ Acute infections, fever, and untreated cancer pose significant risks, making the therapy entirely unsuitable and potentially harmful․
Acute Infections
Applying Manual Lymphatic Drainage (MLD) during an acute infection is strictly contraindicated․ This is because MLD encourages fluid movement throughout the lymphatic system, and attempting to mobilize fluids when the body is actively fighting an infection can inadvertently spread the infection more widely․ The lymphatic system, while crucial for immune function, can become a pathway for disseminating pathogens if stimulated during an acute phase․
Specifically, conditions like acute bronchitis, pneumonia, or even a severe cold or flu represent absolute contraindications․ The body’s resources are entirely focused on localizing and eliminating the infection; introducing lymphatic manipulation could overwhelm the system․ Furthermore, the gentle pressure used in MLD might exacerbate inflammation and discomfort associated with the infection․ It’s vital to allow the body to resolve the infection naturally before considering any lymphatic support therapies․ Post-infection, once the acute phase has passed and the individual is recovering, MLD may be beneficial, but only with careful assessment and practitioner discretion․
Fever
The presence of a fever constitutes a firm contraindication for Manual Lymphatic Drainage (MLD)․ A fever is a systemic response indicating the body is actively combating an underlying illness, often an infection․ Similar to acute infections, manipulating the lymphatic system during a febrile state risks spreading the causative agent throughout the body, potentially worsening the condition and increasing systemic stress․
MLD’s intention is to mobilize fluids, and in a feverish state, this could inadvertently distribute inflammatory mediators and pathogens more rapidly․ The body’s thermoregulatory system is already working overtime; adding the physiological effects of MLD could further destabilize it․ It’s crucial to prioritize allowing the body to regulate its temperature and fight the illness without external intervention․ Deferring MLD until the fever has subsided for at least 24-48 hours, without the use of antipyretics, is essential․ A qualified practitioner will always assess for fever before initiating treatment, prioritizing patient safety above all else․
Acute Thrombophlebitis
Acute thrombophlebitis, characterized by inflammation and clot formation in a vein, is a significant contraindication to Manual Lymphatic Drainage (MLD)․ The gentle, rhythmic movements of MLD, while generally beneficial, can potentially dislodge a thrombus (blood clot) that has formed within the vein․ This dislodged clot could then travel through the circulatory system, leading to a potentially life-threatening pulmonary embolism if it reaches the lungs․
Even in areas seemingly distant from the site of thrombophlebitis, MLD can exert systemic effects that increase the risk of clot mobilization․ The increased circulation stimulated by the therapy isn’t desirable when a clot is present․ A thorough assessment by a healthcare professional is vital to rule out thrombophlebitis before commencing MLD․ Treatment should be postponed until the inflammation has resolved and the clot has stabilized, typically under medical supervision․ Practitioners must prioritize patient safety and avoid any intervention that could exacerbate this serious condition․
Congestive Heart Failure
Congestive Heart Failure (CHF) represents a critical contraindication for Manual Lymphatic Drainage (MLD) due to the compromised cardiovascular system․ Individuals with CHF have a heart unable to pump sufficient blood to meet the body’s needs, leading to fluid buildup․ MLD, by encouraging fluid mobilization through the lymphatic system, can significantly overload an already strained heart․
The increased fluid volume returning to the central circulation, stimulated by MLD, can exacerbate the symptoms of CHF, such as shortness of breath, edema, and fatigue․ The heart may be unable to effectively manage this sudden influx of fluid, potentially leading to acute decompensation․ A careful medical evaluation is essential to determine the severity of CHF and assess the patient’s suitability for any lymphatic therapy․ MLD should be avoided in cases of moderate to severe CHF, and even mild cases require cautious consideration and physician approval before treatment is initiated․ Prioritizing cardiac stability is paramount․
Kidney Failure
Kidney failure, whether acute or chronic, poses a significant contraindication to Manual Lymphatic Drainage (MLD) due to the kidneys’ crucial role in fluid and electrolyte balance․ Impaired renal function diminishes the body’s capacity to effectively process and eliminate excess fluids mobilized by MLD․ This can lead to a dangerous buildup of toxins and fluid overload, exacerbating the existing strain on the compromised kidneys․
MLD’s stimulation of lymphatic flow increases fluid return to the bloodstream, relying on the kidneys to filter and excrete this fluid․ When kidneys are failing, this process is severely hampered; Symptoms like edema, hypertension, and electrolyte imbalances can worsen․ A thorough medical assessment, including kidney function tests, is vital before considering MLD․ In cases of significant renal impairment, MLD is generally contraindicated․ Even with milder kidney dysfunction, careful monitoring and physician oversight are essential to prevent adverse effects and ensure patient safety․
Untreated Cancer
Untreated cancer represents a firm contraindication for Manual Lymphatic Drainage (MLD) due to the potential for inadvertently spreading cancerous cells․ The lymphatic system is a primary pathway for metastasis – the process by which cancer cells disseminate from the primary tumor to other parts of the body․ MLD, by actively encouraging lymphatic flow, could theoretically accelerate this spread, worsening the prognosis․
Even without confirmed metastasis, stimulating the lymphatic system in the presence of an undiagnosed or untreated malignancy carries inherent risks․ It’s crucial to have a definitive cancer diagnosis and a clear treatment plan established before considering MLD․ If cancer treatment is ongoing (surgery, chemotherapy, radiation), MLD may be permissible with physician approval, but always after acute phases․ A detailed medical history, including cancer screening results, is paramount․ Prioritizing cancer management and avoiding any intervention that could potentially compromise treatment outcomes is essential for patient well-being․
Relative Contraindications for MLD
Certain conditions require extra caution with MLD․ These aren’t absolute ‘no-gos’, but demand careful assessment and potential modification of the treatment approach․
Chronic Kidney Disease
Individuals with chronic kidney disease (CKD) necessitate a particularly cautious approach to Manual Lymphatic Drainage (MLD)․ The kidneys play a vital role in fluid balance, and compromised kidney function can significantly impact the body’s ability to manage fluid levels effectively․ MLD, by its nature, mobilizes fluids, potentially overwhelming kidneys already struggling to maintain homeostasis․
Therefore, MLD should only be considered with explicit medical clearance from a nephrologist․ The practitioner must be fully aware of the patient’s kidney function status, including glomerular filtration rate (GFR) and any existing fluid restrictions․ Gentle, proximal techniques are favored, avoiding aggressive or deep work that could exacerbate fluid shifts․
Close monitoring during and after treatment is essential, watching for signs of fluid overload, such as edema or shortness of breath․ MLD may be contraindicated altogether in advanced stages of CKD or if the patient is undergoing dialysis․ Prioritizing patient safety and collaborating with their healthcare team is paramount․
Liver Disease
Patients with liver disease require careful evaluation before undergoing Manual Lymphatic Drainage (MLD)․ The liver is central to fluid balance and protein synthesis – crucial for maintaining oncotic pressure, which prevents fluid leakage into tissues․ Liver dysfunction can disrupt these processes, leading to ascites (fluid accumulation in the abdomen) and edema․
MLD’s fluid mobilization effect could potentially worsen these conditions․ Therefore, MLD should only be performed with explicit approval from the patient’s hepatologist․ The practitioner needs detailed knowledge of the liver disease’s stage, presence of portal hypertension, and any existing fluid restrictions․
Treatment should be exceptionally gentle, focusing on proximal lymphatic pathways and avoiding deep abdominal work․ Monitoring for signs of increased ascites or edema is vital․ MLD might be entirely contraindicated in cases of severe liver failure or decompensated cirrhosis․ Collaboration with the patient’s medical team is essential to ensure safety and avoid adverse effects․
Active Bleeding Disorders
Manual Lymphatic Drainage (MLD) is absolutely contraindicated in individuals with active bleeding disorders․ These conditions, such as hemophilia or thrombocytopenia, compromise the body’s ability to form blood clots, increasing the risk of hemorrhage even with minor trauma․ The gentle, yet purposeful, pressure applied during MLD could inadvertently exacerbate bleeding, internally or externally․
This includes patients currently taking anticoagulant medications (blood thinners) who exhibit uncontrolled bleeding․ Even seemingly innocuous petechiae (small, pinpoint hemorrhages) or easy bruising should prompt a thorough assessment and likely contraindicate MLD․
Prior to treatment, a detailed medical history is paramount to identify any bleeding tendencies․ If a patient has a history of a bleeding disorder, clearance from their hematologist is mandatory․ MLD’s stimulation of circulation, while generally beneficial, could prove dangerous in this context․ Safety is the utmost priority, and avoiding any potential to induce or worsen bleeding is critical․
Recent Thrombosis
Manual Lymphatic Drainage (MLD) is strongly contraindicated following a recent thrombosis – the formation of a blood clot within a blood vessel․ Whether deep vein thrombosis (DVT) or superficial thrombophlebitis, manipulating the area risks dislodging the clot and initiating a potentially life-threatening pulmonary embolism (PE) if it travels to the lungs․
“Recent” generally refers to within the past three to six months, but this timeframe can vary based on the clot’s location, size, and the individual’s overall health․ A physician’s clearance is absolutely essential before considering MLD in these cases․
Even if the acute phase has passed and the patient is on anticoagulation therapy, caution is warranted․ MLD’s circulatory effects could theoretically influence clot stability․ A thorough assessment of the affected limb, including signs of post-thrombotic syndrome, is crucial․ Prioritizing patient safety dictates erring on the side of caution and avoiding MLD until medically cleared․
Post-Surgical Period (Early Stages)
Following surgery, the body undergoes a complex healing process, and Manual Lymphatic Drainage (MLD) is generally contraindicated in the immediate postoperative phase․ This initial period, typically the first few weeks, is characterized by inflammation, tissue disruption, and a fragile vascular network․ Applying MLD too soon can disrupt clot formation essential for wound healing and potentially exacerbate swelling․
The risk of infection is also heightened post-surgery, and MLD, while gentle, could theoretically spread bacteria․ Furthermore, surgical sites often experience compromised lymphatic drainage naturally; aggressive manipulation could overwhelm the system․
The timing for introducing MLD post-surgery depends on the procedure’s extent and the individual’s recovery․ A physician’s approval is paramount, usually after the acute inflammatory phase subsides and the wound begins to close․ Gradual, gentle techniques focused around the surgical site, rather than directly on it, may be considered later in recovery․
Pregnancy
Pregnancy represents a period of significant physiological change, making Manual Lymphatic Drainage (MLD) a treatment requiring careful consideration․ While not an absolute contraindication, MLD during pregnancy necessitates a cautious approach and a thorough understanding of potential effects․
Hormonal shifts during pregnancy cause fluid retention and increased blood volume, potentially altering lymphatic flow․ Stimulating the lymphatic system could, in theory, induce uterine contractions, particularly in the first trimester, although evidence is limited․ Certain lymphatic points are traditionally avoided due to their proximity to uterine nerves․
MLD can be beneficial for managing edema common in pregnancy, but it should only be performed by a therapist specifically trained in prenatal massage and MLD․ A physician’s approval is essential before initiating treatment․ Gentle techniques focused on legs and feet are generally considered safer, while abdominal work is typically avoided․
Pacemakers and Other Implanted Devices
The presence of pacemakers or other implanted medical devices introduces a unique set of considerations regarding Manual Lymphatic Drainage (MLD)․ These devices, crucial for regulating bodily functions, can be susceptible to interference from external forces, including massage techniques․
MLD involves gentle, rhythmic movements that create subtle energy shifts within the body․ While generally safe, these movements could potentially disrupt the function of an implanted device, leading to malfunction or inaccurate readings․ The electromagnetic fields generated during MLD, though minimal, are a theoretical concern․
Direct pressure or manipulation over the device itself is strictly contraindicated․ A qualified MLD therapist must be informed of the device’s location and type․ Treatment should be modified to avoid the area surrounding the implant, maintaining a safe distance․ Physician clearance is absolutely essential before commencing MLD in patients with implanted devices, ensuring a risk-benefit assessment is conducted;

Specific Conditions Requiring Caution
Certain pre-existing health issues necessitate a cautious approach to MLD․ Careful evaluation and potential modification of techniques are vital for patient safety and comfort․
Asthma
Individuals with asthma require careful consideration before undergoing Manual Lymphatic Drainage (MLD)․ While MLD isn’t typically an absolute contraindication, the potential for triggering bronchospasm or exacerbating respiratory symptoms exists․ The gentle, rhythmic movements of MLD can sometimes stimulate the nervous system, which, in sensitive individuals with asthma, might lead to airway constriction․
It’s crucial for the practitioner to be fully aware of the patient’s asthma history, including the severity of their condition, frequency of attacks, and current medication regimen․ A thorough assessment should be conducted to determine the patient’s respiratory status before commencing treatment․ Modifications to the MLD technique may be necessary, such as avoiding deep abdominal work or focusing on areas further away from the chest․
Close monitoring during the session is essential, and the patient should be encouraged to communicate any discomfort or breathing difficulties immediately․ If any respiratory symptoms arise, the treatment should be stopped promptly․ Consulting with the patient’s physician prior to MLD is highly recommended to ensure its safety and appropriateness․
Hypothyroidism
Patients diagnosed with hypothyroidism necessitate a cautious approach to Manual Lymphatic Drainage (MLD)․ This condition, characterized by an underactive thyroid gland, often results in slowed metabolic processes and reduced circulation․ MLD, while generally gentle, can still stimulate the lymphatic and circulatory systems, potentially overwhelming a compromised system․
The primary concern lies in the possibility of exacerbating symptoms like fatigue, fluid retention, and sensitivity to temperature changes; Individuals with hypothyroidism may experience a more pronounced response to lymphatic stimulation, requiring a significantly modified treatment plan․ The practitioner must prioritize gentle techniques and avoid deep or vigorous maneuvers․
Prior to treatment, verifying the patient’s thyroid hormone levels and overall stability is crucial․ Collaboration with the patient’s endocrinologist is highly recommended․ During the session, careful observation for any adverse reactions, such as increased fatigue or swelling, is essential․ MLD should be considered only if the hypothyroidism is well-managed and the patient is stable․
Skin Infections
The presence of any skin infection constitutes a firm contraindication for Manual Lymphatic Drainage (MLD)․ This includes localized infections like cellulitis, impetigo, or fungal infections, as well as widespread conditions such as eczema or psoriasis experiencing active flare-ups․ MLD’s primary action – moving fluids – risks spreading the infection systemically, potentially leading to serious complications․
Lymphatic vessels, while integral to immune function, can inadvertently become pathways for pathogens if the skin barrier is compromised․ Stimulating lymphatic flow in the affected area could accelerate the dissemination of bacteria, viruses, or fungi to previously unaffected tissues․ This could worsen the infection and delay healing․
MLD should only be considered after the infection has completely resolved and the skin barrier is fully intact․ A thorough assessment of the skin’s condition is paramount, and any signs of inflammation, redness, or pus formation necessitate postponing treatment․ Prioritizing infection control and allowing the body to heal naturally is crucial before introducing lymphatic manipulation․
Fragile Capillaries
Individuals with noticeably fragile capillaries require significant caution when considering Manual Lymphatic Drainage (MLD)․ Conditions like telangiectasia (spider veins) or easy bruising indicate compromised capillary integrity, making them susceptible to damage from even gentle pressure; MLD, while typically light-touch, still involves manipulation of superficial tissues, potentially causing capillary rupture and localized bleeding․
The lymphatic system operates in close proximity to the capillary network․ Increasing lymphatic flow can inadvertently increase pressure within the capillaries, exacerbating their fragility․ This risk is heightened in areas with pre-existing capillary damage or thinning skin, common in older adults;
A modified approach, with extremely light pressure and avoidance of areas with visible capillary fragility, might be considered, but only with a thorough assessment and informed consent․ However, in many cases, MLD may be entirely contraindicated; Prioritizing vascular health and avoiding further trauma to delicate capillaries is essential․
Radiation Therapy (Recent)
Recent radiation therapy is a significant contraindication for Manual Lymphatic Drainage (MLD) in the treated area․ Radiation causes significant tissue damage, including inflammation, fibrosis, and compromised vascular integrity․ The skin and underlying tissues become exceptionally sensitive and fragile, increasing the risk of adverse reactions from even gentle manipulation․
MLD’s intent to stimulate lymphatic flow could disrupt the healing process and potentially redistribute inflammatory mediators, exacerbating discomfort and hindering tissue repair․ The irradiated area’s compromised immune response also elevates the risk of infection if the skin barrier is breached during treatment․
A general guideline suggests avoiding MLD for at least 12 months post-radiation, though this timeframe can vary based on the radiation dosage, area treated, and individual healing capacity․ Consultation with the patient’s oncologist is mandatory before considering any lymphatic work in a previously irradiated field․ Prioritizing tissue recovery is paramount․

Important Considerations Before MLD
Thorough evaluation is key․ A detailed medical history and assessment by a qualified practitioner are vital to identify any potential contraindications before treatment․
Medical History Assessment
A comprehensive medical history is the cornerstone of safe and effective Manual Lymphatic Drainage (MLD); Before initiating any treatment, a qualified practitioner must meticulously review the patient’s health background․ This includes identifying pre-existing conditions, current medications, and any recent or ongoing health concerns․
Specifically, the assessment should focus on conditions like acute infections, fever, and active bleeding disorders, as these represent absolute contraindications․ The presence of congestive heart failure, kidney failure, or untreated cancer also necessitates avoiding MLD․ Furthermore, recent thrombosis or being in the early post-surgical period requires careful evaluation․
Relative contraindications, such as chronic kidney disease, liver disease, pregnancy, or the presence of pacemakers, demand a modified approach or outright avoidance depending on the individual case․ Even seemingly minor factors, like fragile capillaries or recent radiation therapy, warrant caution․ A detailed history allows the practitioner to tailor the treatment, if appropriate, or recommend alternative therapies․
Professional Qualification of Practitioner
Selecting a highly trained and qualified practitioner is paramount when considering Manual Lymphatic Drainage (MLD), especially given the importance of understanding contraindications․ MLD is a specialized technique requiring in-depth knowledge of the lymphatic system, anatomy, and physiology – and crucially, when not to apply the therapy․
A competent practitioner will possess specific certification in MLD, demonstrating a thorough understanding of absolute and relative contraindications․ They should be adept at conducting a comprehensive medical history assessment, identifying potential risks, and modifying treatment plans accordingly․ Simply being a general massage therapist is insufficient․
Proper training equips the practitioner to recognize subtle signs that might indicate a contraindication, even if not initially disclosed by the patient․ They will understand the potential consequences of performing MLD on someone with a condition like acute infection or congestive heart failure․ Verification of credentials and experience is essential to ensure patient safety and optimal outcomes․